What is rheumatoid arthritis?
Rheumatoid arthritis, or RA, is a disease that causes pain, swelling, and stiffness in the joints.
RA is one of many different types of arthritis. Its exact cause is still unknown, but we know that factors such as heredity and smoking play a role.
RA is an autoimmune disorder. A disease is called “autoimmune” when a person’s infection-fighting system, called the immune system, “attacks” the body. The body’s immune system mistakenly identifies some normal parts of the body as “foreign,” and so healthy cells are attacked as potentially harmful.
In RA, the immune system attacks the joints. More rarely, it can also attack other parts of the body, such as the lungs, heart, or eyes.
What does a healthy joint look like?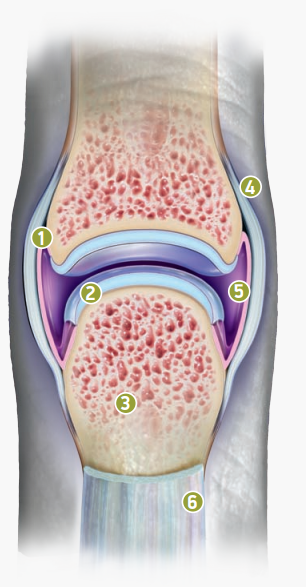
1 Synovial membrane
is the thin layer of tissue that lines the inside of the joint capsule and is the first area affected by RA
2 Articular cartilage
helps reduce friction between bones during joint movement
3 Bones
are connected by the joint
4 Joint capsule
surrounds the joint for protection and support
5 Synovial fluid
lubricates and nourishes the articular cartilage and bones inside
the joint capsule
6 Tendons and ligaments
help support the joint
What are the symptoms of RA?
The main symptom is pain and swelling in the joints.
Different types of arthritis can cause similar symptoms.
However, there are some signs that are more characteristic of inflammatory arthritis such as RA. For example:
- People with RA have more severe joint stiffness in the early hours of the day, which usually improves with movement as the day progresses. Other types of arthritis tend to cause more severe stiffness in patients towards the end of the day or throughout the day.
- RA usually starts by affecting the small joints of the fingers and toes, wrists, and ankles. It usually affects both the left and right sides of the body.
How is RA treated?
It is treated by a doctor who specializes in RA, called a “rheumatologist.” If a patient is diagnosed with RA, they need to start treatment immediately. Early treatment can help prevent many complications. There are many different medications for RA.
 Medications for treating RA are called disease-modifying antirheumatic drugs, or “DMARDs.”
Medications for treating RA are called disease-modifying antirheumatic drugs, or “DMARDs.”
It may take several weeks (6-8 weeks) of taking DMARDs before the patient feels better.
To treat the inflammation in the meantime, other medications may be given for a short period of time, such as:
- Steroids (cortisone) – These can be taken either as a pill or as an injection into a swollen joint.
- Nonsteroidal anti-inflammatory drugs or “NSAIDs”
Most people do not need stronger painkillers, called “opioids.” Unlike other medications, opioids do not help with inflammation or joint damage.
Treatment initially involves conventional DMARDs such as methotrexate (pills or subcutaneous injection), leflunomide, and others.
If this treatment is not sufficient or there are side effects, biological agents (biological DMARDs) or targeted synthetic DMARDs may be administered.
Patients suffering from RA may also be helped by other health professionals, such as:
● Physical therapist (exercise specialist) 
Movement can be painful for patients with RA.
A physical therapist can help patients understand which types of activities are best for them and incorporate them into their daily routine.
● Occupational therapist
Helps patients find ways to continue performing their normal daily tasks despite the functional problems they may have due to RA. Can create special splints for patients if certain joints are too painful or non-functional.
The goal of occupational therapists is to help individuals lead independent, productive, and fulfilling lives.
● Nutritionist
Maintaining a healthy body weight and getting the necessary nutrients is very important.
Weight loss helps obese individuals feel better, as carrying excess weight puts additional strain on the joints.
● Cardiologist/Internist/General Practitioner
People with rheumatoid arthritis are more likely to develop heart problems.
It is very important to keep blood pressure, cholesterol, and blood sugar under control, and smokers should quit smoking. It is essential that patients work closely with a cardiologist, internist, or general practitioner to control these factors.
● Rheumatism Association and Mental Health Specialist
It is normal for a patient who discovers they have rheumatoid arthritis to initially feel anxious, upset, and sad.
Many patients find it helpful to talk to other people who are going through similar issues. The Association of Rheumatism Sufferers of Crete, as well as other associations for rheumatism sufferers, provide a suitable environment for patients to feel understood and supported.
Sometimes, negative feelings can be more intense. In these cases, it is helpful to visit a mental health professional (psychologist or psychiatrist) to talk or even take medication, when necessary.
What can I do on my own?
● Stay active
The patient may want to avoid physical activity because it hurts. However, this will make things worse as the muscles will become weaker and the joints stiffer than they already are.
 Staying active can help the patient feel less tired and have less pain. It can also help them sleep better.
Staying active can help the patient feel less tired and have less pain. It can also help them sleep better.
Walking, swimming, and Pilates with proper guidance can be suitable activities as they do not strain the joints, but at the same time help strengthen muscles, maintain joint mobility, and improve cardiorespiratory endurance.
● Eat a healthy diet
People with rheumatoid arthritis are at risk of heart disease, so it is important to avoid foods high in saturated fat. Instead, it is important to eat plenty of fruits, vegetables, and foods rich in omega-3 fatty acids.
● Stop smoking
Smoking further increases the risk of heart disease.
What if I want to get pregnant?
It is possible for a patient with RA to have a safe, healthy pregnancy. It is essential to consult with your doctor before attempting to conceive, as:
● Some of the medications used to treat RA are not safe for a developing fetus. The patient may need to change medications before becoming pregnant.
●There are tests that need to be done before pregnancy to prevent problems during pregnancy.
RA symptoms often improve significantly during pregnancy, but may worsen again after childbirth.
In summary, better cooperation between doctor and patient leads to better treatment outcomes, which in turn improves the quality of life of patients with rheumatic diseases, which is the ultimate goal.



